GLP-1 agonists: treating weight loss with diabetes medication
GLP-1 medications like Wegovy and Saxenda can help reduce hunger and support lasting weight loss. They work best alongside small, sustainable shifts to how you eat, move and feel – with expert support from a programme like Oviva, funded by the NHS.
If you’re living with a BMI over 35 and certain health conditions, you can ask your GP if you’re eligible.
Get our simple info pack for everything you need to book an appointment and start your journey.
Key Takeaways
- GLP-1 agonist medications are used as weight loss and diabetes medication.
- These medications work by suppressing your appetite and reducing food intake.
- GLP-1 medications may be available via NHS prescription, if you meet the criteria.
- The medication should be supported by wider lifestyle interventions, carried out through a specialist weight loss programme like Oviva.

Table of Contents
What are GLP-1 agonist medications and how do they work?
How much weight can I lose with GLP-1 medication?
Are GLP-1 medications right for me?
How can I get a GLP-1 prescription from my GP?
Additional benefits of taking weight loss medications
What are GLP-1 agonist medications and how do they work?
GLP-1 agonists are a class of medications that mimic the effects of a hormone called glucagon-like peptide-1 (GLP-1). This hormone is naturally released after eating and helps to regulate blood glucose levels, while increasing feelings of fullness and delivering an appetite suppression effect. Therefore, GLP-1 agonists serve as both weight loss and diabetes medication.
This appetite suppression effect naturally reduces the amount of food you eat. As you consume fewer calories and combine this with wider lifestyle changes, you lose weight.
There are a number of GLP-1 agonists approved for use in the UK as either weight loss or diabetes medication. The currently approved medications in this category are:
- Semaglutide (Wegovy for weight loss, Ozempic for type 2 diabetes)
- Liraglutide (Saxenda for weight loss, Victoza for type 2 diabetes)
- Tirzepatide (Mounjaro for type 2 diabetes; the NHS approved Mounjaro for weight loss in 2024 but NHS access is still very limited)
- Exenatide (Bydureon, for type 2 diabetes)
- Lixisenatide (Lyxumia, for type 2 diabetes)
- Dulaglutide (Trulicity, for type 2 diabetes)
These medications may be available in tablet or injectable form. Injectable GLP-1 agonists are more common and these can be self-administered at home.

How much weight can I lose with GLP-1 medication?
Clinical studies have demonstrated that GLP-1 agonists are effective for promoting weight loss. In a 2022 study on the effects of semaglutide for weight loss (Rubino et al.) the average weight loss for participants receiving semaglutide and lifestyle interventions was 15.7% over 68 weeks. Other GLP-1 agonists have also been shown to promote weight loss of 10% or more.
Are GLP-1 weight loss medications right for me?
GLP-1 medications most commonly treat type 2 diabetes, but studies of semaglutide demonstrated the effectiveness of using this diabetes drug for weight loss. Since then, further studies have helped to demonstrate the use of other GLP-1 agonists for weight loss, including liraglutide and tirzepatide, and this works even in people who do not have diabetes.
GLP-1 medications may be recommended for people with a BMI of 35 or higher, especially if they have at least one other linked medical condition, like asthma, high blood pressure, sleep apnoea or depression.
Weight loss medication of this kind can be especially useful if you’ve previously struggled to lose weight using conventional methods, like dieting and increasing physical activity. When supported with wider lifestyle interventions, the medication can produce excellent results.
Oviva patient success stories:

 -22kg
-22kg
Heidi (53)

 -25kg
-25kg
Martin (34)

 -32kg
-32kg
Patricia (53)

How can I get a GLP-1 prescription from my GP?
If you meet the criteria, you may be eligible for a GLP-1 prescription via the NHS. You can speak to your GP about your weight loss options, including your suitability for GLP-1 weight loss injections.
If you’re eligible, you will be referred to a specialist weight management service, like Oviva. As part of this programme, you’ll receive a tailored weight loss plan, plus medication (if appropriate).
Do I need to have type 2 diabetes to get a GLP-1 prescription for weight loss?
No, you do not need to have type 2 diabetes to receive a prescription for a weight loss medication. However, type 2 diabetes is one of several medical conditions that may make you eligible for a specialist weight management programme if you also have a BMI over 35. Other examples of relevant medical conditions include:
- High blood pressure
- Sleep apnoea
- Depression
- Asthma
- Heart disease
- Polycystic ovary syndrome (PCOS)
- Pre-diabetes
Additional benefits of taking weight loss medications
Weight loss medications may bring other health benefits, outside of weight loss. These can include:
- Reducing blood pressure
- Improving cholesterol
- Lowering the risk of cardiovascular disease
Moreover, they’re relatively easy to administer, as they come in injectable or oral forms, taken either once daily or once weekly. The injectable form can be self-administered at home and will come as a pre-filled pen, so you will not see the needle.
Overall, weight loss medications can be a valuable tool to help you to achieve weight loss goals, improve overall health and reduce the risks of obesity-related health conditions.

What are the potential side effects of weight loss medications?
Like all medications, GLP-1 medications have potential side effects. Most of these side effects are relatively mild and your dosage will be increased gradually to limit the prevalence and severity of side effects. The most common side effects to be aware of are:
- Nausea
- Vomiting
- Diarrhoea
- Constipation
- Stomach pain
Less common and more serious side effects include pancreatitis (inflammation of the pancreas) and allergic reactions. Both of these are regarded as medical emergencies and you should seek urgent medical help if you experience severe abdominal pain or allergy-like symptoms.
Who is not suitable for GLP-1 medications?
GLP-1 medications are not suitable if you’re pregnant, actively trying to become pregnant or currently breastfeeding. If you take a GLP-1 weight loss or diabetes medication, you should stop at least two months before you plan to become pregnant.
If you have diabetes, you may still be able to take a GLP-1 diabetes drug for weight loss, but there are additional considerations. For instance, it could increase the risk of hypoglycaemia (blood glucose levels falling too low).
You should not take GLP-1 weight loss medication alongside other weight loss medications or if you’ve previously displayed symptoms of an allergy to GLP-1s.
How to take GLP-1 agonists
In the following sections, you’ll find useful information on how to take GLP-1 agonists.
How often do you take GLP-1 medications?
GLP-1 medications come in different forms, but the most common is a self-injectable pen. These medications, including Wegovy and Saxenda, are taken once per week and self-administered.
Dosage instructions for GLP-1 agonists
The dosage instructions for GLP-1 medications vary depending on the specific drug and your individual needs. You should receive relevant information from healthcare professionals.
As part of the Oviva programme, you’ll receive support as you gradually increase your dosage, eventually reaching the maintenance dose. This gradual increase allows your body to adapt to the medication more easily and helps to control side effects.
If I take a higher dosage of GLP-1s, will I lose more weight?
Increasing your dosage, up until the established maintenance dose for the GLP-1 medication you’re receiving, has been linked with increased weight loss. However, you should never exceed the recommended maintenance dose and you should gradually reach the maintenance dose over several weeks.
How to inject GLP-1 medications
GLP-1 medications can be self-administered with a pre-filled pen. You’ll be advised on proper injection technique when you begin your treatment.
You can inject into your stomach, the front of your thighs or your upper arms, with the stomach being the recommended location.
You can inject into the same area (e.g. stomach) every time, but you should change the precise injection site to avoid skin reactions. The pre-filled pens are easy to use and you will not see the needle. This helps to make the injections suitable for as many people as possible.

What’s Oviva’s approach?
Oviva’s NHS-funded programme combines expert care with personalised support – all delivered remotely.
- Led by specialists – including dietitians, psychologists and nurses
- Tailored plans – with GLP-1 medication when appropriate
- Long-lasting change – building habits that make a difference now and in the future
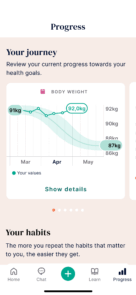
- Progress tracking – via our easy-to-use app
People lose an average of 13.6kg in 12 months – and 97% would recommend us.